High flow oxygen at home12/12/2023 
Oxygen loss is negligible, but, with these devices, high concentrations of oxygen are not available. These devices monitor delivered oxygen concentration, supplied via a low-pressure system, in the delivered gas. High flow can thus be generated even though air and high-pressure oxygen wall supplies are unavailable. These usually use turbines and entrain room air to generate high flow. Precise flow generators are incorporated into devices manufactured by Fisher & Paykel Healthcare (Auckland, New Zealand) and Vapotherm (NH). In general, air-oxygen blenders titrate oxygen concentration according to the amount of medical gas inhaled some gas is lost via the blender. Use of air and oxygen directly from the wall supply, a mechanical air-oxygen blender, and a flow meter enables stable delivery both of F IO 2 and gas flow. Of these, the air-oxygen blender with flow meter is the most popular. There are 3 types of standalone flow generators: air-oxygen blenders, built-in flow generators, and entrainment systems ( Fig. 24 Below, the advantages and disadvantages of each element are discussed separately. 23 As described above, HFNC is a simple system composed of a flow generator, humidifying device, inspiratory limb, and nasal interface ( Fig. HFNC may make it easier to initiate earlier respiratory support, and the device has the potential to decrease the necessity or duration of mechanical ventilation. 18, 19 The simplicity and excellent patient tolerance of the system is attractive, 21 and, owing to these advantages, 16, 22 the use of HFNC for adults who are critically ill has been dramatically increasing. 17– 20 Because HFNC is an open system, it does not actively enhance tidal volume however, it does improve alveolar ventilation by washing out anatomic dead space. 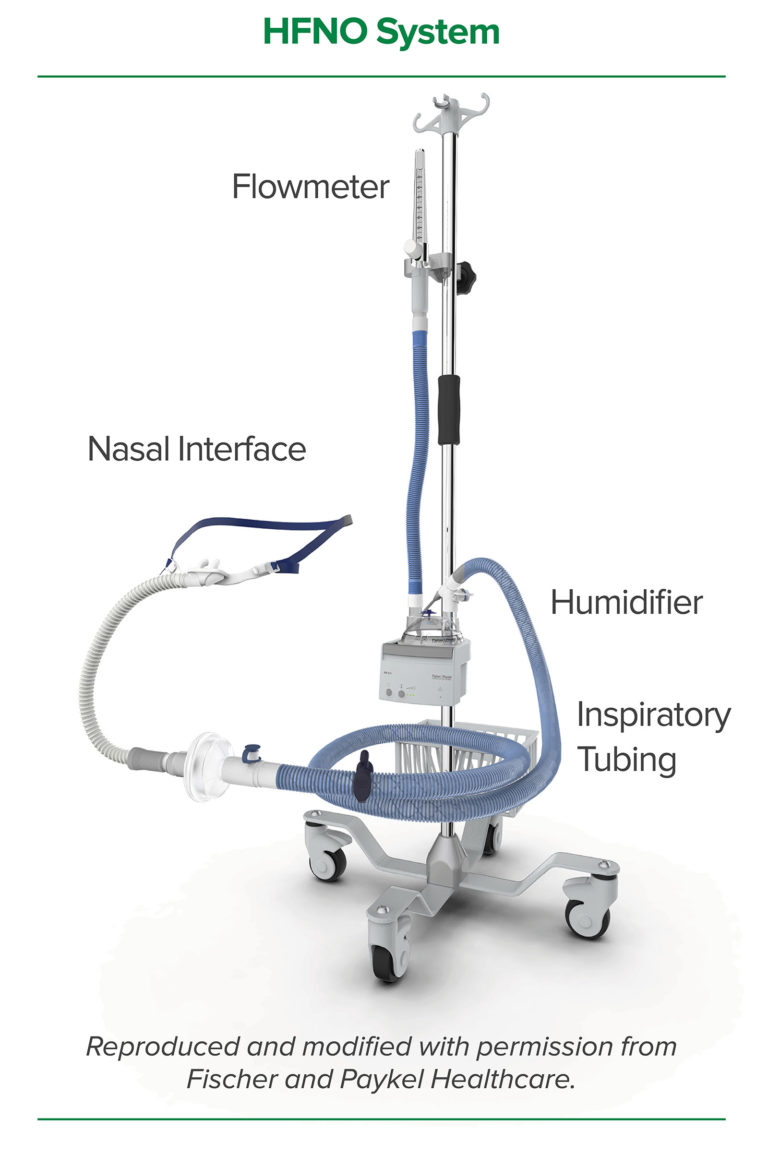
Although NIV interfaces add to the anatomic dead space, HFNC delivery actually decreases dead space. The differences between NIV and HFNC are the interfaces as well as consistent pressure versus the ability to provide different inspiratory and expiratory pressures. 16 According to the monitored oxygen concentration, F IO 2 can be titrated with flows up to 60 L/min. 13– 15Ī typical HFNC system consists of a flow generator, active heated humidifier, single-limb heated circuit, and nasal cannula. Analysis of the results of recent clinical trials, however, show that, at least it is not inferior to NIV. 9– 12 Initially, there was skepticism as to whether it was as good as NIV for treating acute hypoxemic respiratory failure. 6– 8 In the 2000s, high-flow nasal cannula (HFNC) therapy gained attention as an alternative means of respiratory support for patients who were critically ill and was attractive because it was even less invasive. 2 Since then, NIV has been found to be superior to invasive ventilation for patients with COPD exacerbations 3, 4 and acute cardiogenic pulmonary edema, 5 in those patients who are immunocompromised and in acute respiratory failure. During the 1990s, physicians began to prescribe noninvasive ventilation (NIV) to support patients with acute respiratory failure. Since then, despite having well-known adverse effects, mechanical ventilation with an endotracheal tube (invasive ventilation) has no doubt saved many patients. In 1967 “acute respiratory distress” was recognized and reported for the first time in the medical literature, 1 and PEEP was considered to be effective for improving oxygenation. For now, although functional differences among the different HFNC systems seem to be minor, to avoid adverse clinical events, it is essential to know the advantages and disadvantages of each element.įor hypoxemic respiratory failure, the frontline treatment is supplemental oxygen. Although the use of HFNC in adults who are critically ill has been dramatically increasing, the advantages and disadvantages of each element have not been well discussed. While NIV interfaces add to anatomic dead space, HFNC delivery actually decreases dead space. The HFNC system is simple: it requires only a flow generator, active heated humidifier, single heated circuit, and nasal cannula. In the 2000s, less invasive high-flow nasal cannula (HFNC) therapy gained attention as an alternative means of respiratory support for patients who were critically ill. During the 1990s, noninvasive ventilation was found to be superior to invasive ventilation for exacerbations of COPD, acute cardiogenic pulmonary edema, and acute respiratory failure in patients who were immunocompromised. Since ARDS was first described, mechanical ventilation via an endotracheal tube (invasive ventilation) has no doubt saved many patients. 
For hypoxemic respiratory failure, the frontline treatment is supplemental oxygen.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
